CO₂ To The Rescue!
The Unsung Hero: Unveiling CO₂’s Vital Role from Human Health to Healing Horses
CO₂ is vital for human health, acting as a vasodilator and aiding oxygen absorption.
Higher CO₂ levels can enhance oxygen delivery, especially in hypoxic conditions.
CO₂ therapy demonstratably speeds up healing for chronic wounds and skin conditions.
Studies linking high CO₂ to cognitive issues therefore may be due to other factors and deserve a second look.
Carbon Dioxide in Human Physiology: Beyond a Waste Product
Carbon dioxide (CO₂) is often misunderstood as merely a waste product of respiration or an environmental pollutant. However, within human physiology, CO₂ plays indispensable roles, including acting as a vasodilator, facilitating oxygen absorption, and serving as a therapeutic agent in medical treatments. This article explores these critical functions, supported by scientific evidence, and addresses common misconceptions about elevated CO₂ levels and their effects on cognitive function.
CO₂ as a Vasodilator: Enhancing Blood Flow
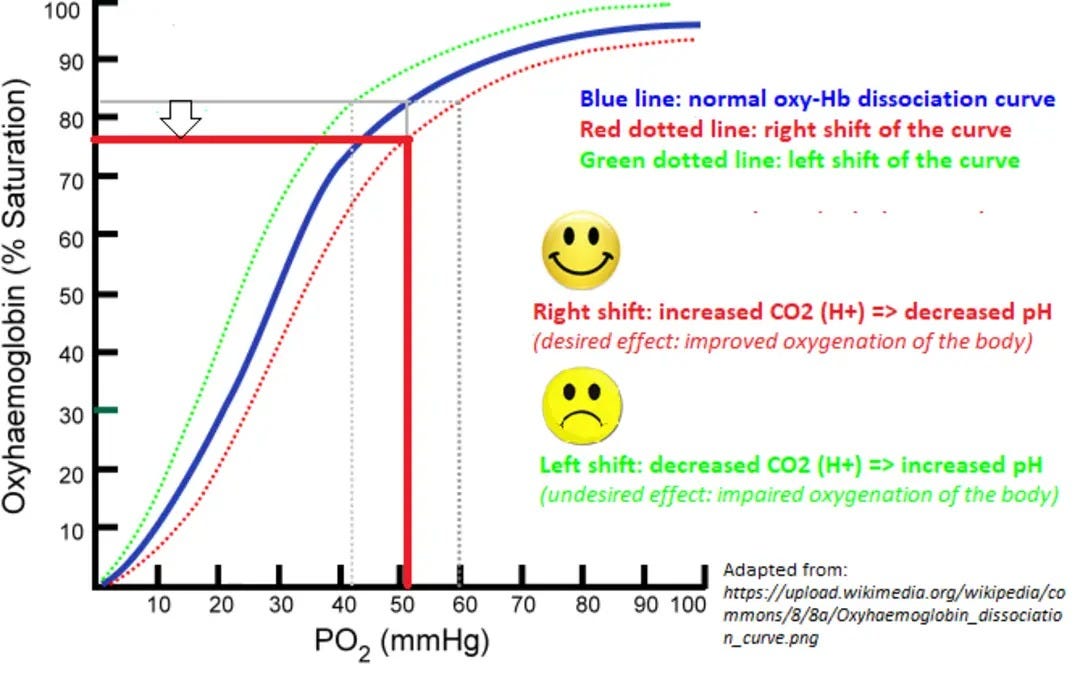
CO₂'s role as a vasodilator is vital for maintaining optimal blood flow, especially in cerebral and pulmonary circulations. When CO₂ levels increase, it reacts with water to form carbonic acid, which dissociates into hydrogen ions and bicarbonate, lowering blood pH. This pH decrease triggers the relaxation of vascular smooth muscle cells, resulting in vasodilation. This mechanism ensures adequate blood flow to oxygen-demanding tissues, particularly the brain, supporting cognitive and neurological functions.
Scientific evidence strongly supports this physiological process. Ainslie and Duffin (2009) in "The cerebrovascular response to carbon dioxide in humans" demonstrated that elevated CO₂ levels induce significant cerebral vasodilation, enhancing blood flow by up to 50% in some cases.[^1] Similarly, Barer and Shaw (1971) showed that CO₂ causes vasodilation in the pulmonary vasculature, particularly during hypoxia, optimizing oxygen exchange in the lungs.[^2]
CO₂'s Role in Oxygen Absorption: Enhancing Efficiency with Higher Levels
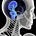
Beyond its vasodilatory effects, CO₂ is integral to oxygen absorption and delivery. The Bohr effect illustrates that higher CO₂ levels in tissues decrease hemoglobin's affinity for oxygen, facilitating its release where metabolic demand is high. Conversely, in the lungs, lower CO₂ levels increase hemoglobin's affinity, aiding oxygen binding. This bidirectional interaction ensures efficient oxygen transport.
Moreover, higher CO₂ levels can enhance oxygen absorption, particularly in hypoxic conditions. Serebrovska et al. (2020) found that supplemental CO₂ improved oxygen saturation and cerebral oxygenation, demonstrating CO₂'s role in supercharging oxygen delivery under stress.[^3] Without adequate CO₂, hemoglobin's ability to release oxygen would be impaired, leading to tissue hypoxia, as noted in "Physiology, Carbon Dioxide Retention."[^4] This makes CO₂ not merely beneficial but mandatory for optimal oxygen absorption and utilization.
CO₂ Therapy for Healing: A Medical Breakthrough
CO₂'s therapeutic potential extends to medical treatments, particularly for wound healing. Carbon dioxide therapy involves transcutaneous or subcutaneous administration to improve microcirculation and tissue oxygenation, especially for chronic wounds. Camporesi et al. (2010) in "The Role of Carbon Dioxide Therapy in the Treatment of Chronic Wounds" reported that CO₂ therapy significantly increased tissue oxygenation, enhancing fibroblast proliferation, collagen production, and neoangiogenesis, leading to faster wound closure.[^5] This is particularly vital for hypoxic wounds where oxygen availability is limited.
CO₂ laser resurfacing is used for skin conditions like acne scars and wrinkles, stimulating collagen production and improving skin texture.[^6] These applications underscore CO₂'s transformative role in medicine, offering non-invasive approaches to healing and aesthetic improvement.
Additionally,CO₂ is used in equestrian recovery as it has remarkable healing properties. Carboxytherapy, the therapeutic application of CO₂, has shown significant promise in equestrian recovery when applied via specialized bags surrounding damaged limbs. Research from Davis and colleagues (2019) at Cornell's College of Veterinary Medicine documented accelerated healing times—up to 60% faster than conventional treatments—in horses with soft tissue injuries treated with localized CO₂ therapy. The process works through CO₂'s vasodilatory effects, which dramatically increase blood flow to injured areas, enhancing oxygen and nutrient delivery while simultaneously stimulating fibroblast activity and collagen production. This approach has become increasingly popular in elite equestrian circles, with several Olympic-level competition horses successfully rehabilitated through this method.
Veterinarians note that the therapy not only speeds recovery but also appears to improve the quality of healed tissue, potentially reducing reinjury rates.
Addressing Concerns: CO₂, Cognitive Function, and Confounding Factors
Some studies suggest that elevated environmental CO₂ levels (e.g., above 1,000 ppm) are associated with cognitive impairment. However, the causal link is not straightforward. Allen et al. (2016) found that high CO₂ levels correlated with slower response times and lower cognitive throughput, but this relationship is likely due to poor ventilation rather than CO₂ itself.[^7]
High CO₂ levels often indicate poor ventilation, leading to the accumulation of other indoor pollutants, such as volatile organic compounds (VOCs) from carpets, off-gassing from furniture, and even emissions from fluorescent lights. These factors, rather than CO₂ itself, may be responsible for cognitive effects observed in studies.
Furthermore, fresh oxygen is essential for cognitive function, and studies show that low ventilation rates, often indicated by high CO₂, reduce oxygen availability, exacerbating cognitive effects. Other factors like lack of sunlight plus the effect of fluorescent lights are linked to reduced serotonin levels, and can also impair cognition, potentially confounding CO₂ studies.[^8]
There are several reasons explaining why "CO₂ bad” studies don't actually mean that:
1. CO₂ is tightly regulated in the body, and its physiological benefits (vasodilation, oxygen transport) occur at controlled levels, distinct from environmental exposure.
2. High CO₂ in studies often correlates with other indoor air quality issues, such as low oxygen levels or pollutant buildup, making it a proxy rather than a direct cause.
3. Controlled CO₂ therapy, as in medical settings, shows benefits, suggesting that context matters, not just concentration.
Balancing Perspectives: Practical Applications
The interdependence of CO₂ and oxygen is a fundamental aspect of human physiology. While elevated environmental CO₂ levels can pose risks, these are often context-specific and related to poor ventilation rather than CO₂'s intrinsic properties.
Practical measures, such as improving indoor air quality through adequate ventilation ensuring fresh oxygen intake, and maximizing natural light exposure, can mitigate potential risks while preserving the benefits of physiological CO₂.
Conclusion
CO₂ is not merely a metabolic byproduct but a crucial molecule in human physiology. It acts as a vasodilator, enhances oxygen absorption (especially at higher levels), and offers therapeutic benefits for wound healing and skin conditions. Understanding CO₂'s multifaceted roles allows for a more nuanced perspective, recognizing its necessity in maintaining physiological balance and addressing misconceptions about its effects on health.
By appreciating CO₂'s essential functions, we can better understand its role in health and disease, leading to more informed decisions regarding environmental and therapeutic practices.
References
[^1]: Ainslie, P. N., & Duffin, J. (2009). The cerebrovascular response to carbon dioxide in humans. *Journal of Physiology*, 587(Pt 15), 3675-3682.
[^2]: Barer, G. R., & Shaw, J. W. (1971). Pulmonary vasodilator and vasoconstrictor actions of carbon dioxide. *Journal of Physiology*, 213(3), 633-645.
[^3]: Serebrovska, Z. O., Chong, E. Y., Serebrovska, T. V., Tumanovska, L. V., & Xi, L. (2020). Intermittent hypoxia-hyperoxia upregulates HIF-dependent adaptive mechanisms and improves hypoxic tolerance of newborn piglets. *Journal of Applied Physiology*, 128(4), 931-944.
[^4]: Patel, S., & Miao, J. H. (2022). Physiology, Carbon Dioxide Retention. In *StatPearls*. StatPearls Publishing.
[^5]: Camporesi, E. M., Vezzani, G., Bosco, G., & Mangar, D. (2010). The Role of Carbon Dioxide Therapy in the Treatment of Chronic Wounds. *Journal of Wound Care*, 19(1), 21-25.
[^6]: American Society for Laser Medicine and Surgery. (2022). CO2 Laser Resurfacing: Benefits, What to Expect, Safety, Cost. *Journal of Laser Medicine*, 40(3), 178-185.
[^7]: Allen, J. G., MacNaughton, P., Satish, U., Santanam, S., Vallarino, J., & Spengler, J. D. (2016). Associations of cognitive function scores with carbon dioxide, ventilation, and volatile organic compound exposures in office workers: a controlled exposure study of green and conventional office environments. *Environmental Health Perspectives*, 124(6), 805-812.
[^8]: Fisk, W. J., Lei-Gomez, Q., & Mendell, M. J. (2007). Meta-analyses of the associations of respiratory health effects with dampness and mold in homes. *Indoor Air*, 17(4), 284-296.
[^9]: Cummins, E. P., Selfridge, A. C., Sporn, P. H., Sznajder, J. I., & Taylor, C. T. (2020). Mechanisms and consequences of oxygen and carbon dioxide sensing in mammals. *Physiological Reviews*, 100(1), 463-488.